What exactly is a
Neurodermatitis?
A skin disease that affects a significant proportion of the global population. It manifests itself through intense itching, redness and skin lesions, which often leads to considerable discomfort and an impaired quality of life for those affected. However, neurodermatitis is not contagious.
Atopic dermatitis often occurs in childhood and can last a lifetime or recur. Relapses can be triggered by stress, allergies or environmental factors. Although there is no cure, symptoms can be effectively treated and controlled.
About the symptoms
More information
Important facts about neurodermatitis
Symptoms and consequences of neurodermatitis:
- Intense itching that leads to scratching and rubbing
- Dry skin condition, often with scaling
- Intense redness and inflammation of the skin
- Weeping of the skin, sometimes with blistering
- Burning and possibly pain in the damaged areas of skin
- Thickening of the skin (lichenification)
- The skin is very sensitive and tends to tear
- Sleep disturbances due to itching
- Mental stress such as anxiety and depression
- Impairment of quality of life due to constant discomfort
Where does atopic dermatitis occur?
Neurodermatitis can manifest itself differently on the skin depending on the age group.
- Infants and young children: Neurodermatitis in infants and young children is characterized by red, scaly patches of skin, particularly on the face (cheeks, forehead), scalp and diaper area. Weeping blisters may appear, accompanied by severe itching. Scratch marks are often visible.
- Childhood and puberty: In this age group, atopic dermatitis occurs more frequently in skin folds such as the bends of the elbows, hollows of the knees, neck or wrists.
- Adults: Neurodermatitis can occur in adults both in the known areas (elbows, hollows of the knees, neck, wrists) and in other parts of the body. In addition, the symptoms often also occur on the face, hands or feet. If the disease persists for a long time, the skin often thickens (lichenification).
What are atopic stigmata?
Atopic stigmata are certain physical characteristics or changes that can occur in people with atopic diseases such as neurodermatitis. They are regarded as possible accompanying symptoms or indications of a genetic predisposition to atopic diseases.
- Dennie Morgan sign (double lower eyelid crease)
- White dermographism (pallor of the skin on mechanical stimulation)
- Hertoghe's sign (thinning of the outer eyebrows)
- Fur cap-shaped hairline (deep lateral hairline on the face)
- Ichthyosis and hyperlinearity on hands and feet (dry skin, wrinkling)
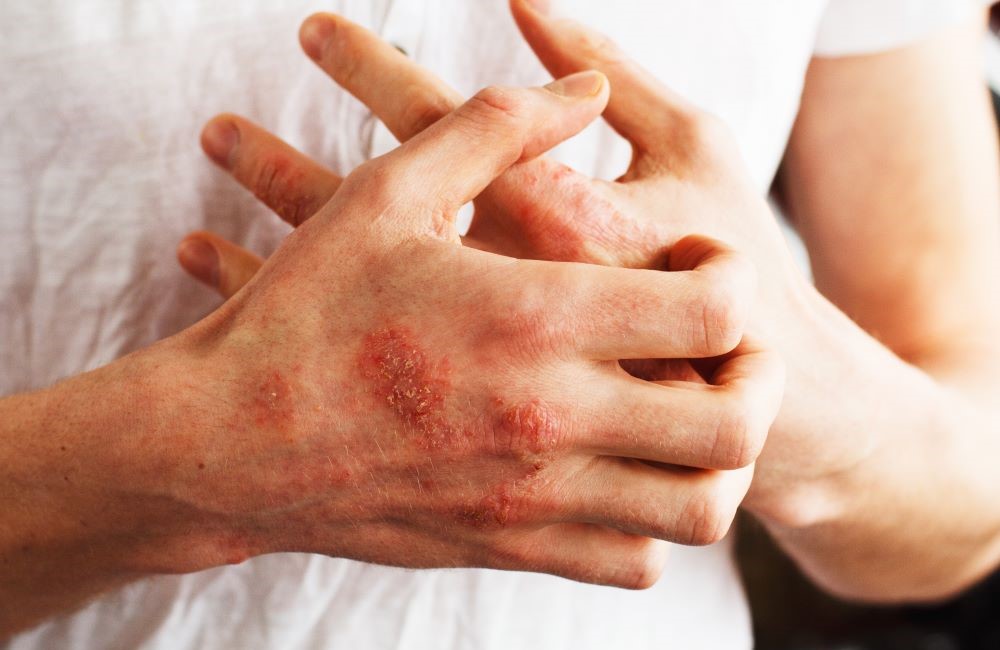
- Hand eczema/foot eczema (skin inflammation on hands/feet, redness, keratinization)
- Atopic facial pallor with periorbital shadow (ring-shaped darkening of the skin around the eyes)
- Keratosis pilaris ("chafing skin", rough skin nodules)
What causes neurodermatitis?
The exact cause of atopic dermatitis is not yet fully understood. However, it is assumed that a combination of genetic predisposition, malfunction of the immune system and environmental factors play a role. However, each case can be individual, with different factors interacting.
The following factors can trigger atopic dermatitis or exacerbate a flare-up:
Genetic predisposition
Genetic predisposition
Family predisposition to neurodermatitis, asthma or hay fever
Immune system dysfunction
Immune system dysfunction
Overactive activity and sensitivity to certain stimuli
Barrier disorder of the skin
Barrier disorder of the skin
Increased water loss and dryness facilitate the penetration of allergens, irritants and bacteria
Environmental factors
Environmental factors
Allergens e.g. pollen, house dust mites, animal hair, certain foods;
Irritating substances e.g. cleaning agents, fragrances, extreme temperatures
Lifestyle and psychological factors
Lifestyle and psychological factors
e.g. stress, emotional strain, unhealthy lifestyle
How is atopic dermatitis diagnosed?
Neurodermatitis is usually diagnosed by a dermatologist. It is recommended to consult a doctor if symptoms occur that indicate atopic dermatitis and persist, worsen or impair the quality of life.
Medical history and recording of symptoms
Clinical examination for redness, skin lesions, dryness, thickening and atopic stigmata
Exclusion of other causes such as allergic reactions, infections or other skin diseases

Sources
Please note that all content provided regarding individual medical conditions, treatments, procedures, etc. is general information and may vary depending on the physician:in and individual case and initial situation.
For more detailed information, please always consult your doctor.
Association of the Scientific Medical Societies in Germany: Neurodermatitis
www.awmf.orgRobert Koch Institute: Allergic diseases in children and adolescents in Germany - cross-sectional results from KiGGS wave 2 and trends. Journal of Health Monitoring
www.rki.deWerfel Thomas, Deutsche Dermatologische Gesellschaft Aberer Werner, Österreichische Gesellschaft für Dermatologie und Venerologie Ahrens Frank, Gesellschaft für Pädiatrische Allergologie und Umweltmedizin e.V., et al: Ärztliche Leitlinie Neurodermitis.
Deutsche Haut- und Allergiehilfe e.V.: Neurodermitis – Ursachen und Auslöser; unter: www.dha-neurodermitis.de
European Centre for Allergy Research Foundation (ECARF): "Neurodermatitis"
www.ecarf.orgLangan SM, Irvine AD, Weidinger S. Atopic dermatitis. Lancet 2020; 396(10247): 345-360.